Post Herpetic Neuralgia can be like a Spear in the Chest
It Can Be Prevented – But at a Price
Shingles is a virus that resides in nerve roots near the spinal cord. It is activated by aging, most commonly over age 60. A shingles episode lasts approximately three weeks. However, one out of six people will experience nerve pain that lasts a month after the rash is gone, and a few (3%) will experience Post-Herpetic Neuralgia for a year or more. The pain is where the rash had been. It can be as bad as the worst pain you’ve ever had at the dentist – but 24 hours a day without relief. The “spear through the chest” description was given to me by a patient many years ago. He could barely sleep, eat, wear clothing, or function. His PHN formed a band on one side of his chest. He said if it were on his leg, he would consider cutting the leg off.
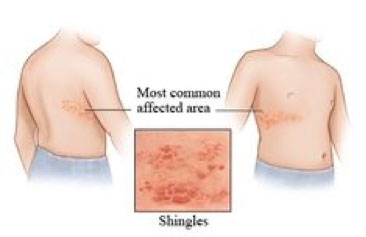
1 out of every 3 people in the United States will develop shingles, also known as herpes zoster, in their lifetime. There are an estimated 1 million cases of shingles each year in this country. Anyone who has recovered from chickenpox may develop shingles; even children can get shingles. By age 85, approximately 50% of the population will develop shingles. Vaccination is the only way to protect against shingles.
The new shingles vaccine is bothersome, expensive, and causes discomfort at the injection site 75% of the time (think of the old tetanus shot). But most patients agree that if one can avoid shingles and PHN, the injection discomfort will be worth it. To help you make an informed decision with your doctor, I have provided the Center for Disease Control description of the vaccine.
—#—
(CDC) The recombinant zoster vaccine (brand name Shingrix) is a two-dose vaccine that is more than 90% protective against shingles, even among the elderly. CDC recommends that immunocompetent adults aged 50 years and older receive two doses of Shingrix, with the second dose given 2 -6 months after the first dose. Shingrix must be administered intramuscularly (for example, in the deltoid region of the upper arm). This is very important because if Shingrix is administered subcutaneously, the patient is more likely to develop an injection-site reaction with pain, redness, or swelling.
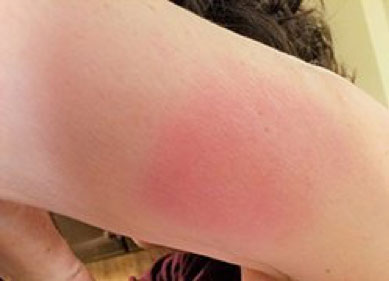
Figure 1: Pain, redness, and swelling from an incorrectly administered Shingrix vaccination.
Modest local and systemic reactions to Shingrix are quite common. The clinical trials of Shingrix and reports to the Vaccine Adverse Event Reporting System (VAERS) have provided a detailed picture of reactions to this vaccine. In eight clinical trials of more than 10,000 people who completed reaction diaries, 78% of those who got Shingrix reported some pain at the injection site, 38% reported redness, and 26% reported swelling. For 1%-3% people, the area of redness and swelling exceeded 4 inches.
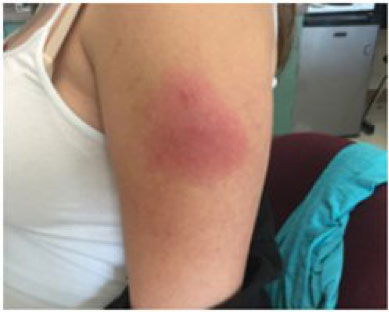
Figure 2: Redness even when Shingrix was administered correctly. Discomfort is minor.
In addition to local reactions, about 1 in 10 people who received Shingrix in clinical trials reported systemic effects such as muscle pain, fatigue, headache, shivering, fever, or gastrointestinal illness.
From October 2017 to June 2018, healthcare providers and patients have submitted just over 4000 reports to VAERS of events involving Shingrix. About 3.2 million doses of Shingrix were distributed during that timeframe. The most common symptoms reported to VAERS were fever, injection-site pain, and redness. Reassuringly, the results of early monitoring of Shingrix are consistent with the safety profile observed in clinical trials; serious adverse events were rare, and no unusual patterns were detected; almost all reactions resolved in 3 days.
For more information, visit CDC’s shingles vaccine website.
—#—
Web Resources
Shingles Vaccine Information for Healthcare Professionals
Conclusion:
The vaccine is in short supply due to great demand from those over 70. That is the largest demographic to have experienced or witnessed shingles and PHN. They think the marginally greater discomfort and redness of the vaccine is worth avoiding the disease. If you are planning on living past 70, you might consider this. That is your cost/benefit equation.